Podcast: Play in new window | Download (Duration: 4:02 — 8.0MB)
Subscribe: RSS
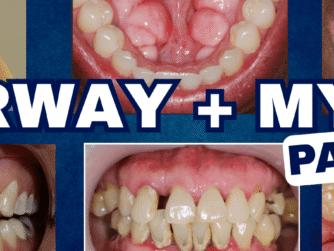
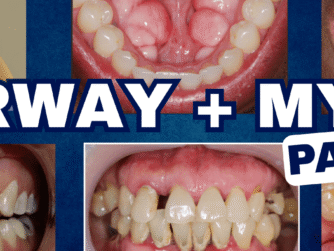
After the cliffhanger from Part 1, Dr. Sandra Hulac is back to share more information about Frictional and Constricted Chewing Patterns (CCP) with cases shared and explanations given.
Check out the Full Episode with a Free membership on Protrusive.App
Download Protrusive App on iOS and Android and Claim your Verifiable CPD/CE by answering a few questions + You can get EARLY ACCESS to the episode + EXCLUSIVE content
The Protrusive Dental Pearl: Overjet is King. We don’t want tight bites. We want a bit of overjet that gives chewing space – this will reduce the chances of a functional attrition and avoid ‘too much anterior guidance’ or locking the patient in.
“It’s important to know why things fail and try and avoid failure the next time”
Highlights of this episode:
- 0:28 PDP141 – Stop Blaming Bruxism Part 1 Recap
- 6:34 The Protrusive Dental Pearl: Overjet is King
- 6:56 The role of pre-restorative orthodontics
- 9:24 Case #1: Extremely traumatic deep bite
- 14:10 Case #2: Crowding of the lower anterior segment
- 19:41 Case #3 Lot of wear on the front teeth
- 23:54 Case #4: Chipped and worn front teeth
- 27:06 Case #5: Worn front teeth
- 32:41 Case #6: Patient had an extraction ortho
Dr. Mahmoud and I are also excited to share the occlusion that we learned over the years – in a way that you have never seen before!
Occlusion: Basics and Beyond is the most tangible, real-world, and comprehensive occlusion training on the planet.
LIMITED DELEGATE SPOTS DUE TO STARTER KIT STOCK – AVOID DISAPPOINTMENT! Occlusion Online Course
Be sure to watch Part 1: Stop Blaming Bruxism! How to Spot Frictional and Constricted Chewing Patterns (CCP)

Continuing Education Information
This activity may be eligible for continuing education credit through Protrusive Guidance. Participants must complete the associated quiz inside Protrusive Guidance to obtain CPD certification.
Cost:
Access to this CE activity is included with an active Protrusive Guidance membership. Current membership pricing is available at
www.protrusive.app.
Cancellation & Refund Policy:
Memberships may be cancelled at any time. Access to CE activities remains active until the end of the current billing cycle. Subscription charges are non-refundable once processed. Full details are available at
www.protrusive.app.